There are millions of osteoarthritis (OA) sufferers around the world and the OA treatment market is worth more than $3.5 billion annually. However, despite this, treatment relies heavily on generic drugs, many of which focus on reducing pain and inflammation rather than addressing the causes and processes of the disease. There are precious few drugs available, or even in development, that modify and control OA, especially at its later stages.
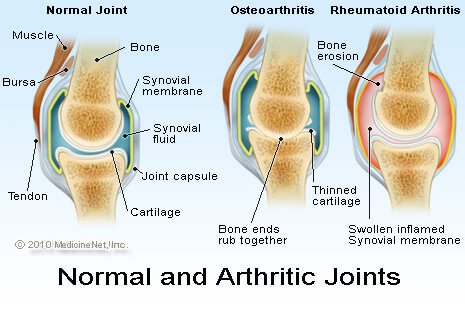
Osteoarthritis (OA or Degenerative Arthritis)
The cost of failed drugs is estimated to run into many billions, so what will help us in our fight against this painful and debilitating condition? New technologies, including Bitplane’s 3D image analysis software and genetic medicine, may come to our aid.

How You Can (and Can’t) Help a Loved One Struggling with Addiction
Patient phenotyping is a possible solution

Seeing the World from a Different Perspective
One of the problems with OA is that its causes are still poorly understood, so choosing the right candidates for different drug trials is very hit-and-miss. Selecting trial candidates according to phenotype – in this case how the disease manifests – is one route that’s being looked at.
The suggested phenotypes for patients and their disease manifestations are:
- chronic pain which involves central nervous system mechanisms;
- mainly inflammatory arthritis;
- metabolic diseases and disturbances like diabetes, obesity and others;
- alterations in bone and cartilage metabolism;
- mainly mechanical arthritis, and
- minimal disease causing slight symptoms with very slow progression.
The fact that there are different phenotypes suggests that there are several causes and underlying mechanisms leading to the disease. Research is focussing on the two main areas where patient needs are unmet – pain relief and the slowing down of joint degeneration. Pain relief drugs don’t slow down the disease, in fact some may speed up its progression as joints are made more comfortable to use. It’s important, therefore, to match up the phenotype to the right drug trials to tackle to root causes of the OA and to gain greater evidence of efficacy.
Defining efficacy and progress is essential

Don’t Forget Dignity: Give Your Aging Relative Some Personal Space
OA presents problems when it comes to efficacy endpoints, too. Pain is a very subjective thing, so patient-reported outcomes aren’t reliable. On top of this, placebo effects in OA drug trials tend to be very strong and persistent. Even more concrete measurables like structure modification are hampered by the fact that OA often has an irregular progression. This is one area where imaging will be able to offer definitive proof of efficacy – or indeed the lack of. Longer clinical trials may be the answer here, as well as more sophisticated sub-set selection combined with the more objective and sensitive imaging tech.
The role of imaging

Will We Be Using Digital Pathologists Soon?
Measuring efficacy in OA still relies too much on just X-rays to mark the changes in joints. However, MRI can examine not just the bones, but the cartilage, the menisci and the synovium, as well as other soft and connective tissues that make up the joint. It’s becoming increasingly clear that the more sensitive imaging methods, like MRI, are better able to detect and understand the changes, including progression and (hopefully) improvement, in OA.